Do you find yourself asking these questions?
A healthy woman of reproductive age has a vaginal pH of around 4, but the pH undergoes significant changes during different stages of their life as hormone levels change (figure 2) :
- Pre-menstruation: pH 7.0
- Reproductive-age: pH 3.8–4.4
- Menopause: pH 6.5–7.0 (without hormone therapy)
pH 4.5–5.0 (with hormone replacement therapy)
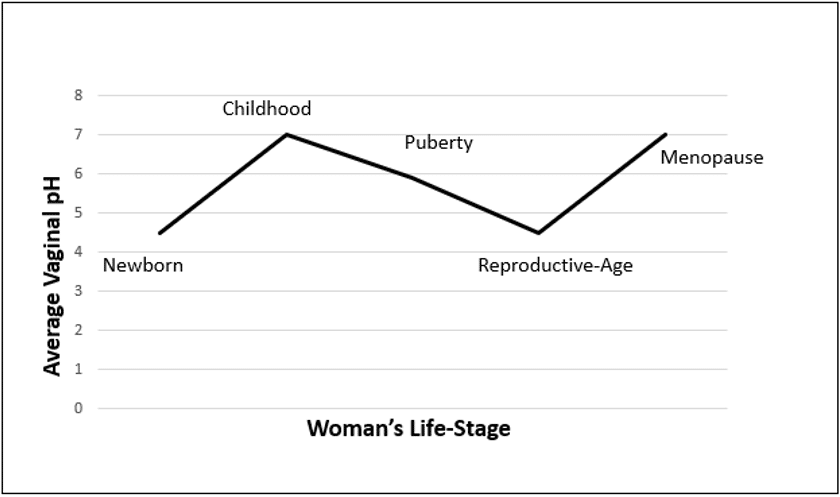
Adapted from Kale & Ubgade 2013
Figure 1. pH and life-stage
Changes in vaginal pH can occur as a result of a range of common life-stage and lifestyle ‘pH triggers’ including:
- Puberty and adolescence
- Menstruation
- Pregnancy
- Menopause
- Sexual activity
- Douching, cleansers and feminine hygiene
- Vaginal irritation
- Vaginal itching and burning
- Thin, watery, grey vaginal discharge
- Unpleasant vaginal colour (fishy odour)
There are a range of ‘self-help’ actions women can undertake to help maintain a healthy vaginal pH and prevent potential vulvovaginal problems — guideline recommendations on female genital hygiene include:
- Undertaking daily intimate hygiene to keep genital area clean
- Using a hypoallergenic, mild liquid wash (pH 4.2 to 5.6); avoiding abrasive bar soaps or more alkaline bath products and irritants
- Not using fragranced vaginal douches
- Wearing loose-fitting cotton underwear; changing underwear frequently; minimising the wearing of tight clothes
- Not using talcum powder and only the sparing use of perfumes and deodorants
- Changing tampons and other sanitary items frequently
- Gently cleansing the vulva (from front to back) before and after intercourse; not irrigating the vagina
- Avoiding any sensitivity or scarring when removing pubic hair
- Using lactic acid-based products with an acidic pH may help with skin homeostasis and may be helpful in vaginal infections as adjuvant therapy (not as a treatment).
Vaginal dryness is a very common problem which is caused by a lack of natural moisture inside the vagina. Itching, irritation and discomfort are also very common and tend to occur as a result of long term dryness.
Vaginal dryness occurs during and after menopause but can also occur as a result of:
- Childbirth
- Breastfeeding
- Oral contraceptives
- Immune disorders
- Chemotherapy
- Hormone therapy
- At times of stress
Oestrogen helps keep the vagina moist and maintains the thickness of the vaginal lining. Vaginal dryness happens when the ovaries produce a decreased amount of oestrogen. This can occur at certain times in a woman’s life, and may be permanent or temporary. Whenever oestrogen levels remain low (as they naturally do after menopause), the entire vaginal area tends to be dry both inside and out, which can lead to itching, irritation and discomfort.
Allergy and cold medications, as well as some antidepressants, can decrease the moisture in many parts of the body, including the vagina.
- Pain and discomfort during intercourse
- Vaginal itching
- Vaginal burning
There are treatments that can help restore or ease vaginal dryness. These include personal lubricants and vaginal moisturisers.
- Use lubricants to ease pain during intercourse.
- Vaginal moisturisers (Aci-Jel Restore) can help to improve vaginal dryness.
Both are products at your local pharmacy without a prescription.
Talk to your doctor if you’re going through menopause; there are a range of treatments available, and your doctor will be able to determine the correct solution for you.